Addressing Pes Planus
Overview

The appearance of flat feet is normal and common in infants, partly due to "baby fat" which masks the developing arch and partly because the arch has not yet fully developed. The human arch develops in infancy and early childhood as part of normal muscle, tendon, ligament and bone growth. Training of the feet, especially by foot gymnastics and going barefoot on varying terrain, can facilitate the formation of arches during childhood, with a developed arch occurring for most by the age of four to six years. Flat arches in children usually become proper arches and high arches while the child progresses through adolescence and into adulthood. A survey of 297 suburban school children up to the age of 10 years at Allahabad in U.P. in India revealed 40.32% children under 5 years, 22.15% children between 5-10 years and 15.48% children above 10 years but below 15 years having bilateral flat foot.
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
A significant number of people with fallen arches (flat feet) experience no pain and have no problems. Some, however, may experience pain in their feet, especially when the connecting ligaments and muscles are strained. The leg joints may also be affected, resulting in pain. If the ankles turn inwards because of flat feet the most likely affected areas will be the feet, ankles and knees. Some people have flat feet because of a developmental fault during childhood, while others may find that the problem develops as they age, or after a pregnancy. There are some simple devices which may prevent the complications of flat feet.
Diagnosis
You can always give yourself the ?wet test? described above to see whether you have flat feet. Most people who do not notice their flat feet or have no pain associated with them do not think to see a foot doctor. Flat feet can lead to additional problems such as stiffness or pain, however, especially if the condition appears out of nowhere. If you think you may have flat feet, you should seek medical attention to ensure there are no additional issues to worry about. Your doctor will be able to diagnose you with a number of tests. For example, he or she may have you walk around, stand still, or stand on your tiptoes while you are being examined. Your doctor may also examine your foot?s shape and functionality. It?s important to let your foot doctor know about your medical and family history. In some cases, your doctor may order imaging tests such as x-rays or an MRI (magnetic resonance imaging) to determine a cause of your flat foot. If tarsal coalition is suspected in children, a CT scan is often ordered.
arch supports for high arches
Non Surgical Treatment
If you have fallen arches, but you are not experiencing any symptoms, then you probably do not need to seek treatment. If you are experiencing discomfort due to fallen arches, there are several treatment options. These treatment options include elevating the feet and applying ice to ease discomfort and reduce swelling, rest, exercises to stretch the feet, physical therapy, medication, such as anti-inflammatories, steroid injections and orthotic devices or customised arch supportsto wear in the shoes. If you have fallen arches and periodically experience pain related to that condition, it is a good idea to get orthotic devicesor custom arch supports, to wear in your shoes. The other treatment options, like medication and ice, will help to ease pain from fallen arches after you have already begun to experience pain. However, orthotic devices or(custom arch supports)can help to prevent pain from occurring at all. This preventative measure helps many people with fallen arches to avoid pain and prevent worsening of their condition. In severe cases of fallen arches, surgery may be required to correct the problem. You can also help to prevent pain and exacerbation of fallen arches by reducing your risk factors. If you are overweight, try to lose weight. Even a small weight loss can reduce the pressure on your feet significantly. If you are diabetic, manage your blood sugar as best as possible. Losing weight often also improves the condition of diabetics. You should also avoid high-impact activities, like running on the road, tennis, and sports that involve jumping. Try a gentler form of exercise, like swimming, instead. If you have fallen arches, orthotic devices or(custom arch supports)are an important component of your treatment and can help to prevent pain.
Surgical Treatment

Surgical correction is dependent on the severity of symptoms and the stage of deformity. The goals of surgery are to create a more functional and stable foot. There are multiple procedures available to the surgeon and it may take several to correct a flatfoot deformity. Stage one deformities usually respond to conservative or non-surgical therapy such as anti-inflammatory medication, casting, functional orthotics or a foot ankle orthosis called a Richie Brace. If these modalities are unsuccessful surgery is warranted. Usually surgical treatment begins with removal of inflammatory tissue and repair of the posterior tibial tendon. A tendon transfer is performed if the posterior tibial muscle is weak or the tendon is badly damaged. The most commonly used tendon is the flexor digitorum longus tendon. This tendon flexes or moves the lesser toes downward. The flexor digitorum longus tendon is utilized due to its close proximity to the posterior tibial tendon and because there are minimal side effects with its loss. The remainder of the tendon is sutured to the flexor hallucis longus tendon that flexes the big toe so that little function is loss. Stage two deformities are less responsive to conservative therapies that can be effective in mild deformities. Bone procedures are necessary at this stage in order to recreate the arch and stabilize the foot. These procedures include isolated fusion procedures, bone grafts, and/or the repositioning of bones through cuts called osteotomies. The realigned bones are generally held in place with screws, pins, plates, or staples while the bone heals. A tendon transfer may or may not be utilized depending on the condition of the posterior tibial tendon. Stage three deformities are better treated with surgical correction, in healthy patients. Patients that are unable to tolerate surgery or the prolonged healing period are better served with either arch supports known as orthotics or bracing such as the Richie Brace. Surgical correction at this stage usually requires fusion procedures such as a triple or double arthrodesis. This involves fusing the two or three major bones in the back of the foot together with screws or pins. The most common joints fused together are the subtalar joint, talonavicular joint, and the calcaneocuboid joint. By fusing the bones together the surgeon is able to correct structural deformity and alleviate arthritic pain. Tendon transfer procedures are usually not beneficial at this stage. Stage four deformities are treated similarly but with the addition of fusing the ankle joint.

The appearance of flat feet is normal and common in infants, partly due to "baby fat" which masks the developing arch and partly because the arch has not yet fully developed. The human arch develops in infancy and early childhood as part of normal muscle, tendon, ligament and bone growth. Training of the feet, especially by foot gymnastics and going barefoot on varying terrain, can facilitate the formation of arches during childhood, with a developed arch occurring for most by the age of four to six years. Flat arches in children usually become proper arches and high arches while the child progresses through adolescence and into adulthood. A survey of 297 suburban school children up to the age of 10 years at Allahabad in U.P. in India revealed 40.32% children under 5 years, 22.15% children between 5-10 years and 15.48% children above 10 years but below 15 years having bilateral flat foot.
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
A significant number of people with fallen arches (flat feet) experience no pain and have no problems. Some, however, may experience pain in their feet, especially when the connecting ligaments and muscles are strained. The leg joints may also be affected, resulting in pain. If the ankles turn inwards because of flat feet the most likely affected areas will be the feet, ankles and knees. Some people have flat feet because of a developmental fault during childhood, while others may find that the problem develops as they age, or after a pregnancy. There are some simple devices which may prevent the complications of flat feet.
Diagnosis
You can always give yourself the ?wet test? described above to see whether you have flat feet. Most people who do not notice their flat feet or have no pain associated with them do not think to see a foot doctor. Flat feet can lead to additional problems such as stiffness or pain, however, especially if the condition appears out of nowhere. If you think you may have flat feet, you should seek medical attention to ensure there are no additional issues to worry about. Your doctor will be able to diagnose you with a number of tests. For example, he or she may have you walk around, stand still, or stand on your tiptoes while you are being examined. Your doctor may also examine your foot?s shape and functionality. It?s important to let your foot doctor know about your medical and family history. In some cases, your doctor may order imaging tests such as x-rays or an MRI (magnetic resonance imaging) to determine a cause of your flat foot. If tarsal coalition is suspected in children, a CT scan is often ordered.
arch supports for high arches
Non Surgical Treatment
If you have fallen arches, but you are not experiencing any symptoms, then you probably do not need to seek treatment. If you are experiencing discomfort due to fallen arches, there are several treatment options. These treatment options include elevating the feet and applying ice to ease discomfort and reduce swelling, rest, exercises to stretch the feet, physical therapy, medication, such as anti-inflammatories, steroid injections and orthotic devices or customised arch supportsto wear in the shoes. If you have fallen arches and periodically experience pain related to that condition, it is a good idea to get orthotic devicesor custom arch supports, to wear in your shoes. The other treatment options, like medication and ice, will help to ease pain from fallen arches after you have already begun to experience pain. However, orthotic devices or(custom arch supports)can help to prevent pain from occurring at all. This preventative measure helps many people with fallen arches to avoid pain and prevent worsening of their condition. In severe cases of fallen arches, surgery may be required to correct the problem. You can also help to prevent pain and exacerbation of fallen arches by reducing your risk factors. If you are overweight, try to lose weight. Even a small weight loss can reduce the pressure on your feet significantly. If you are diabetic, manage your blood sugar as best as possible. Losing weight often also improves the condition of diabetics. You should also avoid high-impact activities, like running on the road, tennis, and sports that involve jumping. Try a gentler form of exercise, like swimming, instead. If you have fallen arches, orthotic devices or(custom arch supports)are an important component of your treatment and can help to prevent pain.
Surgical Treatment

Surgical correction is dependent on the severity of symptoms and the stage of deformity. The goals of surgery are to create a more functional and stable foot. There are multiple procedures available to the surgeon and it may take several to correct a flatfoot deformity. Stage one deformities usually respond to conservative or non-surgical therapy such as anti-inflammatory medication, casting, functional orthotics or a foot ankle orthosis called a Richie Brace. If these modalities are unsuccessful surgery is warranted. Usually surgical treatment begins with removal of inflammatory tissue and repair of the posterior tibial tendon. A tendon transfer is performed if the posterior tibial muscle is weak or the tendon is badly damaged. The most commonly used tendon is the flexor digitorum longus tendon. This tendon flexes or moves the lesser toes downward. The flexor digitorum longus tendon is utilized due to its close proximity to the posterior tibial tendon and because there are minimal side effects with its loss. The remainder of the tendon is sutured to the flexor hallucis longus tendon that flexes the big toe so that little function is loss. Stage two deformities are less responsive to conservative therapies that can be effective in mild deformities. Bone procedures are necessary at this stage in order to recreate the arch and stabilize the foot. These procedures include isolated fusion procedures, bone grafts, and/or the repositioning of bones through cuts called osteotomies. The realigned bones are generally held in place with screws, pins, plates, or staples while the bone heals. A tendon transfer may or may not be utilized depending on the condition of the posterior tibial tendon. Stage three deformities are better treated with surgical correction, in healthy patients. Patients that are unable to tolerate surgery or the prolonged healing period are better served with either arch supports known as orthotics or bracing such as the Richie Brace. Surgical correction at this stage usually requires fusion procedures such as a triple or double arthrodesis. This involves fusing the two or three major bones in the back of the foot together with screws or pins. The most common joints fused together are the subtalar joint, talonavicular joint, and the calcaneocuboid joint. By fusing the bones together the surgeon is able to correct structural deformity and alleviate arthritic pain. Tendon transfer procedures are usually not beneficial at this stage. Stage four deformities are treated similarly but with the addition of fusing the ankle joint.
Heel Aches Everything You Might Want To Know Heel Aches
Overview

The most common form of heel pain, is pain on the bottom of the heel. It tends to occur for no apparent reason and is often worse when first placing weight on the foot. Patients often complain of pain the first thing in the morning or after getting up to stand after sitting. The pain can be a sharp, searing pain or present as a tearing feeling in the bottom of the heel. As the condition progresses there may be a throbbing pain after getting off your feet or there may be soreness that radiates up the back of the leg. Pain may also radiate into the arch of the foot.
Causes
Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation maybe aggravated by shoes that lack appropriate support and by the chronic irritation that sometimes accompanies an athletic lifestyle. Achilles Tendinopathy, Pain and inflammation of the tendon at the back of the heel that connects the calf muscle to the foot. Sever?s, Often found in children between the ages of 8 - 13 years and is an inflammation of the calcaneal epiphyseal plate (growth plate) in the back of the heel. Bursitis. An inflamed bursa is a small irritated sack of fluid at the back of the heel. Other types of heel pain include soft tissue growths, Haglunds deformity (bone enlargement at the back of the heel), bruises or stress fractures and possible nerve entrapment.
Symptoms
Sever?s Disease. This is a condition that occurs in 10 - 15 year old children, predominantly boys and is associated with running and repetitive jumping. It is also associated with flimsy footwear that kids may wear. It occurs when the Achilles tendon continually pulls on the apophysis of the calcaneum and does not allow for it to fuse with the body of the calcaneum. Calcaneal enthesopathy. This occurs when there is repetitive trauma at the attachment of the Achilles tendon, resulting in a spur from the calcaneum up into the Achilles tendon. It is usually visualized on x-ray and may be tender if there is an associated bursitis or tendonitis. "Pump Bump". Also known as Haglund?s Deformity, this is a bony enlargement that exists on the back of the heel - usually related to a congenital abnormality or with chronic bursitis, causing a thickening. There may have already been trauma or pressure from footwear. Treatment is usually protection of the bump and correct footwear. Associated with a symmetrical swelling at the base of the Achilles tendon. It is usually related to repetitive trauma or inappropriate footwear. It is often red and hot in the early stages. Treatment is usually to correct the footwear, provide padding and treat the local symptoms e.g. ice, rest, physiotherapy and cortisone injection. Fat Pad Syndrome. Direct contact with the base of the heel may result in trauma to the fat pad. Related to obesity, training on hard surfaces, uneven grounds, poor shoes especially overlarge shoes which can cause shearing forces on the heel. These conditions are renowned for taking a long time to recover - usually many months.
Diagnosis
Your doctor will listen to your complaints about your heel and examine you to see what is causing the pain, and whether anything else has started it off. If the cause of your pain seems obvious, your doctor may be happy to start treatment straight away. However, some tests may be helpful in ruling out other problems. Blood tests may be done for arthritis. An Xray will show any arthritis in the ankle or subtalar joint, as well as any fracture or cyst in the calcaneum. (It will also show a spur if you have one, but as we know this is not the cause of the pain.) Occasionally a scan may be used to help spot arthritis or a stress fracture.
Non Surgical Treatment
Treatment for plantar fasciitis should be directed at resting the plantar fascia, providing support for the arch area and limiting pronation. This is often accomplished with the use of supportive strapping with athletic tape, arch supports and orthotics. Heel lifts may also be helpful. Anti-inflammatories, pills as well as cortisone injections, may be effective as an adjunctive treatment by speeding up the reduction of inflammation. However, if used alone, anti-inflammatories rarely lead to resolution of the condition. Stretching exercises, physical therapy and night splints may also be helpful. The majority of cases respond to non-surgical treatment although it may take several weeks to reach a comfortable level. In those cases that do not respond adequately to conservative measures, surgical release of the plantar fascia may be considered. However, a new non-surgical treatment called Extracorporeal Shockwave Therapy (ESWT) is now available as an option for recalcitrant plantar fasciitis. ESWT was approved by the FDA recently for the treatment of chronic heel pain. It has been in use for several years on thousands of patients in Europe and has been successfully used to restore patients with chronic plantar fasciitis to a normal, active lifestyle. ESWT is a non-invasive procedure that uses high intensity sound waves similar to what is routinely used to treat kidney stones. The treatment is usually performed in the office or in an outpatient surgical center. The procedure is performed under local anesthesia and takes about 25 minutes. The shockwaves are directed at the plantar fascia and stimulate an inflammatory healing response.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
back of heel cushions
Prevention

Wear properly fitting shoes. Place insoles or inserts in your shoes to help control abnormal foot motion. Maintain a healthy weight. Exercise and do foot stretches as they have been shown to decrease the incidence of heel pain.

The most common form of heel pain, is pain on the bottom of the heel. It tends to occur for no apparent reason and is often worse when first placing weight on the foot. Patients often complain of pain the first thing in the morning or after getting up to stand after sitting. The pain can be a sharp, searing pain or present as a tearing feeling in the bottom of the heel. As the condition progresses there may be a throbbing pain after getting off your feet or there may be soreness that radiates up the back of the leg. Pain may also radiate into the arch of the foot.
Causes
Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation maybe aggravated by shoes that lack appropriate support and by the chronic irritation that sometimes accompanies an athletic lifestyle. Achilles Tendinopathy, Pain and inflammation of the tendon at the back of the heel that connects the calf muscle to the foot. Sever?s, Often found in children between the ages of 8 - 13 years and is an inflammation of the calcaneal epiphyseal plate (growth plate) in the back of the heel. Bursitis. An inflamed bursa is a small irritated sack of fluid at the back of the heel. Other types of heel pain include soft tissue growths, Haglunds deformity (bone enlargement at the back of the heel), bruises or stress fractures and possible nerve entrapment.
Symptoms
Sever?s Disease. This is a condition that occurs in 10 - 15 year old children, predominantly boys and is associated with running and repetitive jumping. It is also associated with flimsy footwear that kids may wear. It occurs when the Achilles tendon continually pulls on the apophysis of the calcaneum and does not allow for it to fuse with the body of the calcaneum. Calcaneal enthesopathy. This occurs when there is repetitive trauma at the attachment of the Achilles tendon, resulting in a spur from the calcaneum up into the Achilles tendon. It is usually visualized on x-ray and may be tender if there is an associated bursitis or tendonitis. "Pump Bump". Also known as Haglund?s Deformity, this is a bony enlargement that exists on the back of the heel - usually related to a congenital abnormality or with chronic bursitis, causing a thickening. There may have already been trauma or pressure from footwear. Treatment is usually protection of the bump and correct footwear. Associated with a symmetrical swelling at the base of the Achilles tendon. It is usually related to repetitive trauma or inappropriate footwear. It is often red and hot in the early stages. Treatment is usually to correct the footwear, provide padding and treat the local symptoms e.g. ice, rest, physiotherapy and cortisone injection. Fat Pad Syndrome. Direct contact with the base of the heel may result in trauma to the fat pad. Related to obesity, training on hard surfaces, uneven grounds, poor shoes especially overlarge shoes which can cause shearing forces on the heel. These conditions are renowned for taking a long time to recover - usually many months.
Diagnosis
Your doctor will listen to your complaints about your heel and examine you to see what is causing the pain, and whether anything else has started it off. If the cause of your pain seems obvious, your doctor may be happy to start treatment straight away. However, some tests may be helpful in ruling out other problems. Blood tests may be done for arthritis. An Xray will show any arthritis in the ankle or subtalar joint, as well as any fracture or cyst in the calcaneum. (It will also show a spur if you have one, but as we know this is not the cause of the pain.) Occasionally a scan may be used to help spot arthritis or a stress fracture.
Non Surgical Treatment
Treatment for plantar fasciitis should be directed at resting the plantar fascia, providing support for the arch area and limiting pronation. This is often accomplished with the use of supportive strapping with athletic tape, arch supports and orthotics. Heel lifts may also be helpful. Anti-inflammatories, pills as well as cortisone injections, may be effective as an adjunctive treatment by speeding up the reduction of inflammation. However, if used alone, anti-inflammatories rarely lead to resolution of the condition. Stretching exercises, physical therapy and night splints may also be helpful. The majority of cases respond to non-surgical treatment although it may take several weeks to reach a comfortable level. In those cases that do not respond adequately to conservative measures, surgical release of the plantar fascia may be considered. However, a new non-surgical treatment called Extracorporeal Shockwave Therapy (ESWT) is now available as an option for recalcitrant plantar fasciitis. ESWT was approved by the FDA recently for the treatment of chronic heel pain. It has been in use for several years on thousands of patients in Europe and has been successfully used to restore patients with chronic plantar fasciitis to a normal, active lifestyle. ESWT is a non-invasive procedure that uses high intensity sound waves similar to what is routinely used to treat kidney stones. The treatment is usually performed in the office or in an outpatient surgical center. The procedure is performed under local anesthesia and takes about 25 minutes. The shockwaves are directed at the plantar fascia and stimulate an inflammatory healing response.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
back of heel cushions
Prevention

Wear properly fitting shoes. Place insoles or inserts in your shoes to help control abnormal foot motion. Maintain a healthy weight. Exercise and do foot stretches as they have been shown to decrease the incidence of heel pain.
Using Heel Lifts For Leg Length Discrepancy
Overview
Surgical lengthening of the shorter extremity (upper or lower) is another treatment option. The bone is lengthened by surgically applying an external fixator to the extremity in the operating room. The external fixator, a scaffold-like frame, is connected to the bone with wires, pins or both. A small crack is made in the bone and tension is created by the frame when it is "distracted" by the patient or family member who turns an affixed dial several times daily. The lengthening process begins approximately five to ten days after surgery. The bone may lengthen one millimeter per day, or approximately one inch per month. Lengthening may be slower in adults overall and in a bone that has been previously injured or undergone prior surgery. Bones in patients with potential blood vessel abnormalities (i.e., cigarette smokers) may also lengthen more slowly. The external fixator is worn until the bone is strong enough to support the patient safely, approximately three months per inch of lengthening. This may vary, however, due to factors such as age, health, smoking, participation in rehabilitation, etc. Risks of this procedure include infection at the site of wires and pins, stiffness of the adjacent joints and slight over or under correction of the bone?s length. Lengthening requires regular follow up visits to the physician?s office, meticulous hygiene of the pins and wires, diligent adjustment of the frame several times daily and rehabilitation as prescribed by your physician.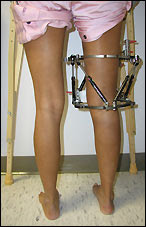
Causes
The causes of LLD may be divided into those that shorten a limb versus those that lengthen a limb, or they may be classified as affecting the length versus the rate of growth in a limb. For example, a fracture that heals poorly may shorten a leg slightly, but does not affect its growth rate. Radiation, on the other hand, can affect a leg's long-term ability to expand, but does not acutely affect its length. Causes that shorten the leg are more common than those that lengthen it and include congenital growth deficiencies (seen in hemiatrophy and skeletal dysplasias ), infections that infiltrate the epiphysis (e.g. osteomyelitis ), tumors, fractures that occur through the growth plate or have overriding ends, Legg-Calve-Perthes disease, slipped capital femoral epiphysis (SCFE), and radiation. Lengthening can result from unique conditions, such as hemihypertrophy , in which one or more structures on one side of the body become larger than the other side, vascular malformations or tumors (such as hemangioma ), which cause blood flow on one side to exceed that of the other, Wilm's tumor (of the kidney), septic arthritis, healed fractures, or orthopaedic surgery. Leg length discrepancy may arise from a problem in almost any portion of the femur or tibia. For example, fractures can occur at virtually all levels of the two bones. Fractures or other problems of the fibula do not lead to LLD, as long as the more central, weight-bearing tibia is unaffected. Because many cases of LLD are due to decreased rate of growth, the femoral or tibial epiphyses are commonly affected regions.
Symptoms
Faulty feet and ankle structure profoundly affect leg length and pelvic positioning. The most common asymmetrical foot position is the pronated foot. Sensory receptors embedded on the bottom of the foot alert the brain to the slightest weight shift. Since the brain is always trying to maintain pelvic balance, when presented with a long left leg, it attempts to adapt to the altered weight shift by dropping the left medial arch (shortening the long leg) and supinating the right arch to lengthen the short leg.1 Left unchecked, excessive foot pronation will internally rotate the left lower extremity, causing excessive strain to the lateral meniscus and medial collateral knee ligaments. Conversely, excessive supination tends to externally rotate the leg and thigh, creating opposite knee, hip and pelvic distortions.
Diagnosis
There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference.
Non Surgical Treatment
Non-surgical treatment can be effective. A shoe lift may be recommended if the leg length difference is less than 1 inch. More significant leg length discrepancies may require a surgical procedure. In children, surgical procedures are available to help make leg lengths more equal.

what is a heel lift?
Surgical Treatment
Surgery is another option. In some cases the longer extremity can be shortened, but a major shortening may weaken the muscles of the extremity. In growing children, lower extremities can also be equalized by a surgical procedure that stops the growth at one or two sites of the longer extremity, while leaving the remaining growth undisturbed. Your physician can tell you how much equalization can be attained by surgically halting one or more growth centers. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the LLD will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical; the goal is to attain equal length of the extremities at skeletal maturity, usually in the mid- to late teens. Disadvantages of this option include the possibility of slight over-correction or under-correction of the LLD and the patient?s adult height will be less than if the shorter extremity had been lengthened. Correction of significant LLDs by this method may make a patient?s body look slightly disproportionate because of the shorter legs.
Surgical lengthening of the shorter extremity (upper or lower) is another treatment option. The bone is lengthened by surgically applying an external fixator to the extremity in the operating room. The external fixator, a scaffold-like frame, is connected to the bone with wires, pins or both. A small crack is made in the bone and tension is created by the frame when it is "distracted" by the patient or family member who turns an affixed dial several times daily. The lengthening process begins approximately five to ten days after surgery. The bone may lengthen one millimeter per day, or approximately one inch per month. Lengthening may be slower in adults overall and in a bone that has been previously injured or undergone prior surgery. Bones in patients with potential blood vessel abnormalities (i.e., cigarette smokers) may also lengthen more slowly. The external fixator is worn until the bone is strong enough to support the patient safely, approximately three months per inch of lengthening. This may vary, however, due to factors such as age, health, smoking, participation in rehabilitation, etc. Risks of this procedure include infection at the site of wires and pins, stiffness of the adjacent joints and slight over or under correction of the bone?s length. Lengthening requires regular follow up visits to the physician?s office, meticulous hygiene of the pins and wires, diligent adjustment of the frame several times daily and rehabilitation as prescribed by your physician.

Causes
The causes of LLD may be divided into those that shorten a limb versus those that lengthen a limb, or they may be classified as affecting the length versus the rate of growth in a limb. For example, a fracture that heals poorly may shorten a leg slightly, but does not affect its growth rate. Radiation, on the other hand, can affect a leg's long-term ability to expand, but does not acutely affect its length. Causes that shorten the leg are more common than those that lengthen it and include congenital growth deficiencies (seen in hemiatrophy and skeletal dysplasias ), infections that infiltrate the epiphysis (e.g. osteomyelitis ), tumors, fractures that occur through the growth plate or have overriding ends, Legg-Calve-Perthes disease, slipped capital femoral epiphysis (SCFE), and radiation. Lengthening can result from unique conditions, such as hemihypertrophy , in which one or more structures on one side of the body become larger than the other side, vascular malformations or tumors (such as hemangioma ), which cause blood flow on one side to exceed that of the other, Wilm's tumor (of the kidney), septic arthritis, healed fractures, or orthopaedic surgery. Leg length discrepancy may arise from a problem in almost any portion of the femur or tibia. For example, fractures can occur at virtually all levels of the two bones. Fractures or other problems of the fibula do not lead to LLD, as long as the more central, weight-bearing tibia is unaffected. Because many cases of LLD are due to decreased rate of growth, the femoral or tibial epiphyses are commonly affected regions.
Symptoms
Faulty feet and ankle structure profoundly affect leg length and pelvic positioning. The most common asymmetrical foot position is the pronated foot. Sensory receptors embedded on the bottom of the foot alert the brain to the slightest weight shift. Since the brain is always trying to maintain pelvic balance, when presented with a long left leg, it attempts to adapt to the altered weight shift by dropping the left medial arch (shortening the long leg) and supinating the right arch to lengthen the short leg.1 Left unchecked, excessive foot pronation will internally rotate the left lower extremity, causing excessive strain to the lateral meniscus and medial collateral knee ligaments. Conversely, excessive supination tends to externally rotate the leg and thigh, creating opposite knee, hip and pelvic distortions.
Diagnosis
There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference.
Non Surgical Treatment
Non-surgical treatment can be effective. A shoe lift may be recommended if the leg length difference is less than 1 inch. More significant leg length discrepancies may require a surgical procedure. In children, surgical procedures are available to help make leg lengths more equal.

what is a heel lift?
Surgical Treatment
Surgery is another option. In some cases the longer extremity can be shortened, but a major shortening may weaken the muscles of the extremity. In growing children, lower extremities can also be equalized by a surgical procedure that stops the growth at one or two sites of the longer extremity, while leaving the remaining growth undisturbed. Your physician can tell you how much equalization can be attained by surgically halting one or more growth centers. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the LLD will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical; the goal is to attain equal length of the extremities at skeletal maturity, usually in the mid- to late teens. Disadvantages of this option include the possibility of slight over-correction or under-correction of the LLD and the patient?s adult height will be less than if the shorter extremity had been lengthened. Correction of significant LLDs by this method may make a patient?s body look slightly disproportionate because of the shorter legs.
Managing Mortons Neuroma
Overview
 A Morton's neuroma usually develops between the third and fourth toes. Less commonly, it develops between the second and third toes. Other locations are rare. It also is rare for a Morton's neuroma to develop in both feet at the same time. The condition is much more common in women than men, probably as a result of wearing high-heeled, narrow-toed shoes. This style of shoe tends to shift the bones of the feet into an abnormal position, which increases the risk that a neuroma will form. Being overweight also increases the risk of a Morton's neuroma.
A Morton's neuroma usually develops between the third and fourth toes. Less commonly, it develops between the second and third toes. Other locations are rare. It also is rare for a Morton's neuroma to develop in both feet at the same time. The condition is much more common in women than men, probably as a result of wearing high-heeled, narrow-toed shoes. This style of shoe tends to shift the bones of the feet into an abnormal position, which increases the risk that a neuroma will form. Being overweight also increases the risk of a Morton's neuroma.
Causes
Some say that this condition should not be called Morton's neuroma as, in fact, it is not actually a neuroma. A neuroma is a non-cancerous (benign) tumour that grows from the fibrous coverings of a nerve. There is no tumour formation in Morton's neuroma. The anatomy of the bones of the foot is also thought to contribute to the development of Morton's neuroma. For example, the space between the long bones (metatarsals) in the foot is narrower between the second and third, and between the third and fourth metatarsals. This means that the nerves that run between these metatarsals are more likely to be compressed and irritated. Wearing narrow shoes can make this compression worse.
Symptoms
If you have a Morton?s neuroma, you may have one or more of these symptoms where the nerve damage is occurring, Tingling, burning, or numbness, pain, a feeling that something is inside the ball of the foot or a feeling that there?s something in the shoe or a sock is bunched up. The progression of a Morton?s neuroma often follows the following pattern. The symptoms begin gradually. At first they occur only occasionally, when wearing narrow-toed shoes or performing certain aggravating activities. The symptoms may go away temporarily by removing the shoe, massaging the foot, or by avoiding aggravating shoes or activities. Over time the symptoms progressively worsen and may persist for several days or weeks. The symptoms become more intense as the neuroma enlarges and the temporary changes in the nerve become permanent.
Diagnosis
A doctor can usually identify Morton's neuroma during a physical exam. He or she will squeeze or press on the bottom of your foot or squeeze your toes together to see if it hurts. Your doctor may also order an X-ray of your foot to make sure nothing else is causing the pain.
Non Surgical Treatment
Anti-inflammatory drugs may be recommended to dull the pain and lessen swelling. Neuropathic pain medications such as the antionvulsants and / or antidepressants may be tried as well. Many are able to recover from this issue at home by icing the area, resting the feet, and by avoiding wearing narrow or tight shoes. If these remedies do not work to alleviate symptoms, the doctor may give special devices to separate the toes and avoid the squeezing of the nerve. Steroid injections may reduce pain and swelling. Surgery may be required if these do not help.
Surgical Treatment
If these non-surgical measures do not work, surgery is sometimes needed. Surgery normally involves a small incision (cut) being made on either the top, or the sole, of the foot between the affected toes. Usually, the surgeon will then either create more space around the affected nerve (known as nerve decompression) or will cut out (resect) the affected nerve. If the nerve is resected, there will be some permanent numbness of the skin between the affected toes. This does not usually cause any problems. You will usually have to wear a special shoe for a short time after surgery until the wound has healed and normal footwear can be used again. Surgery is usually successful. However, as with any surgical operation, there is a risk of complications. For example, after this operation a small number of people can develop a wound infection. Another complication may be long-term thickening of the skin (callus formation) on the sole of the foot (known as plantar keratosis). This may require treatment by a specialist in care of the feet (chiropody).
Prevention
Wearing shoes that fit properly and that have plenty of room in the toe area may help prevent Morton's neuroma.
Causes
Some say that this condition should not be called Morton's neuroma as, in fact, it is not actually a neuroma. A neuroma is a non-cancerous (benign) tumour that grows from the fibrous coverings of a nerve. There is no tumour formation in Morton's neuroma. The anatomy of the bones of the foot is also thought to contribute to the development of Morton's neuroma. For example, the space between the long bones (metatarsals) in the foot is narrower between the second and third, and between the third and fourth metatarsals. This means that the nerves that run between these metatarsals are more likely to be compressed and irritated. Wearing narrow shoes can make this compression worse.
Symptoms
If you have a Morton?s neuroma, you may have one or more of these symptoms where the nerve damage is occurring, Tingling, burning, or numbness, pain, a feeling that something is inside the ball of the foot or a feeling that there?s something in the shoe or a sock is bunched up. The progression of a Morton?s neuroma often follows the following pattern. The symptoms begin gradually. At first they occur only occasionally, when wearing narrow-toed shoes or performing certain aggravating activities. The symptoms may go away temporarily by removing the shoe, massaging the foot, or by avoiding aggravating shoes or activities. Over time the symptoms progressively worsen and may persist for several days or weeks. The symptoms become more intense as the neuroma enlarges and the temporary changes in the nerve become permanent.
Diagnosis
A doctor can usually identify Morton's neuroma during a physical exam. He or she will squeeze or press on the bottom of your foot or squeeze your toes together to see if it hurts. Your doctor may also order an X-ray of your foot to make sure nothing else is causing the pain.
Non Surgical Treatment
Anti-inflammatory drugs may be recommended to dull the pain and lessen swelling. Neuropathic pain medications such as the antionvulsants and / or antidepressants may be tried as well. Many are able to recover from this issue at home by icing the area, resting the feet, and by avoiding wearing narrow or tight shoes. If these remedies do not work to alleviate symptoms, the doctor may give special devices to separate the toes and avoid the squeezing of the nerve. Steroid injections may reduce pain and swelling. Surgery may be required if these do not help.

Surgical Treatment
If these non-surgical measures do not work, surgery is sometimes needed. Surgery normally involves a small incision (cut) being made on either the top, or the sole, of the foot between the affected toes. Usually, the surgeon will then either create more space around the affected nerve (known as nerve decompression) or will cut out (resect) the affected nerve. If the nerve is resected, there will be some permanent numbness of the skin between the affected toes. This does not usually cause any problems. You will usually have to wear a special shoe for a short time after surgery until the wound has healed and normal footwear can be used again. Surgery is usually successful. However, as with any surgical operation, there is a risk of complications. For example, after this operation a small number of people can develop a wound infection. Another complication may be long-term thickening of the skin (callus formation) on the sole of the foot (known as plantar keratosis). This may require treatment by a specialist in care of the feet (chiropody).
Prevention
Wearing shoes that fit properly and that have plenty of room in the toe area may help prevent Morton's neuroma.
For Leg Length Difference Chiropodists Prefer Shoe Lifts
There are not one but two unique variations of leg length discrepancies, congenital and acquired. Congenital indicates you are born with it. One leg is structurally shorter than the other. As a result of developmental stages of aging, the human brain senses the stride pattern and identifies some difference. Our bodies usually adapts by tilting one shoulder over to the "short" side. A difference of less than a quarter inch isn't very irregular, require Shoe Lifts to compensate and ordinarily does not have a serious effect over a lifetime.

Leg length inequality goes typically undiagnosed on a daily basis, however this condition is easily solved, and can eradicate many cases of upper back pain.
Therapy for leg length inequality commonly consists of Shoe Lifts. Most are very reasonably priced, often being below twenty dollars, in comparison to a custom orthotic of $200 or more. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Lower back pain is easily the most common condition impacting people today. Around 80 million men and women are afflicted by back pain at some stage in their life. It is a problem which costs businesses huge amounts of money yearly because of lost time and output. Fresh and more effective treatment solutions are always sought after in the hope of decreasing the economic impact this issue causes.

People from all corners of the earth suffer the pain of foot ache as a result of leg length discrepancy. In these situations Shoe Lifts might be of worthwhile. The lifts are capable of alleviating any discomfort and pain in the feet. Shoe Lifts are recommended by countless skilled orthopaedic physicians.
So that you can support the human body in a healthy and balanced fashion, the feet have a vital function to play. Despite that, it can be the most overlooked region in the human body. Many people have flat-feet which means there may be unequal force placed on the feet. This causes other areas of the body including knees, ankles and backs to be affected too. Shoe Lifts ensure that appropriate posture and balance are restored.

Leg length inequality goes typically undiagnosed on a daily basis, however this condition is easily solved, and can eradicate many cases of upper back pain.
Therapy for leg length inequality commonly consists of Shoe Lifts. Most are very reasonably priced, often being below twenty dollars, in comparison to a custom orthotic of $200 or more. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Lower back pain is easily the most common condition impacting people today. Around 80 million men and women are afflicted by back pain at some stage in their life. It is a problem which costs businesses huge amounts of money yearly because of lost time and output. Fresh and more effective treatment solutions are always sought after in the hope of decreasing the economic impact this issue causes.

People from all corners of the earth suffer the pain of foot ache as a result of leg length discrepancy. In these situations Shoe Lifts might be of worthwhile. The lifts are capable of alleviating any discomfort and pain in the feet. Shoe Lifts are recommended by countless skilled orthopaedic physicians.
So that you can support the human body in a healthy and balanced fashion, the feet have a vital function to play. Despite that, it can be the most overlooked region in the human body. Many people have flat-feet which means there may be unequal force placed on the feet. This causes other areas of the body including knees, ankles and backs to be affected too. Shoe Lifts ensure that appropriate posture and balance are restored.
Shoe Lifts For Leg Length Discrepancy
There are actually not one but two different types of leg length discrepancies, congenital and acquired. Congenital implies that you are born with it. One leg is structurally shorter in comparison to the other. As a result of developmental stages of aging, the brain senses the stride pattern and recognizes some variance. Our bodies usually adapts by dipping one shoulder over to the "short" side. A difference of less than a quarter inch is not grossly uncommon, does not need Shoe Lifts to compensate and generally doesn't have a profound effect over a lifetime.

Leg length inequality goes mainly undiagnosed on a daily basis, however this condition is easily solved, and can eradicate a number of cases of back discomfort.
Therapy for leg length inequality usually consists of Shoe Lifts. These are very inexpensive, in most cases costing below twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lower back pain is the most prevalent ailment impacting people today. Over 80 million people suffer from back pain at some stage in their life. It is a problem which costs companies millions annually because of time lost and production. Innovative and superior treatment methods are always sought after in the hope of lowering economic impact this condition causes.

Men and women from all corners of the earth experience foot ache as a result of leg length discrepancy. In these cases Shoe Lifts can be of very beneficial. The lifts are capable of reducing any discomfort and pain in the feet. Shoe Lifts are recommended by numerous experienced orthopaedic physicians.
So that you can support the body in a well-balanced fashion, feet have got a vital job to play. Inspite of that, it's often the most overlooked region of the human body. Some people have flat-feet meaning there may be unequal force exerted on the feet. This will cause other body parts including knees, ankles and backs to be impacted too. Shoe Lifts guarantee that proper posture and balance are restored.

Leg length inequality goes mainly undiagnosed on a daily basis, however this condition is easily solved, and can eradicate a number of cases of back discomfort.
Therapy for leg length inequality usually consists of Shoe Lifts. These are very inexpensive, in most cases costing below twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lower back pain is the most prevalent ailment impacting people today. Over 80 million people suffer from back pain at some stage in their life. It is a problem which costs companies millions annually because of time lost and production. Innovative and superior treatment methods are always sought after in the hope of lowering economic impact this condition causes.

Men and women from all corners of the earth experience foot ache as a result of leg length discrepancy. In these cases Shoe Lifts can be of very beneficial. The lifts are capable of reducing any discomfort and pain in the feet. Shoe Lifts are recommended by numerous experienced orthopaedic physicians.
So that you can support the body in a well-balanced fashion, feet have got a vital job to play. Inspite of that, it's often the most overlooked region of the human body. Some people have flat-feet meaning there may be unequal force exerted on the feet. This will cause other body parts including knees, ankles and backs to be impacted too. Shoe Lifts guarantee that proper posture and balance are restored.
The Causes Of Calcaneal Spur

Overview
Heel Spurs should be called a traction spurs because they grow in the same direction that the tendons pull away from the heel bone, which is why it can occur on the bottom of the heel (Plantar Fasciitis) and on the back of the heel (Achilles Tendonitis). Some patients may only develop one type of heel spur, but both these problems are closely related so it's not unusual for a patient to have both heel spurs. It's important to note though that most heel spurs aren't the cause of your heel pain.
Causes
Heel spurs form in some patients who have plantar fasciitis (PLAN-tar fash-ee-I-tis), and tend to occur in patients who have had the problem for a prolonged period of time. While about 70 percent of patients with plantar fasciitis have a heel spur, X-rays also show about 50 percent of patients with no symptoms of plantar fasciitis also have a heel spur.

Symptoms
More often than not, heel spurs have no signs or symptoms, and you don?t feel any pain. This is because heel spurs aren?t pointy or sharp pieces of bone, contrary to common belief. Heel spurs don?t cut tissue every time movement occurs; they?re actually deposits of calcium on bone set in place by the body?s normal bone-forming mechanisms. This means they?re smooth and flat, just like all other bones. Because there?s already tissue present at the site of a heel spur, sometimes that area and the surrounding tissue get inflamed, leading to a number of symptoms, such as chronic heel pain that occurs when jogging or walking.
Diagnosis
A Diagnosis of Heel Spur Syndrome is a very common reason for having heel pain. Heel pain may be due to other types of conditions such as tendonitis, Haglund's Deformity, Stress Fracture, Tarsal Tunnel Syndrome, or low back problems. A more common condition in children is Sever's Disease. The diagnosis is usually made with a combination of x-ray examination and symptoms.
Non Surgical Treatment
Treatments for bone spurs and plantar fasciitis include Stretching the calf muscles several times daily is critical in providing tension relief for the plantar fascia. Some physicians may recommend using a step to stretch, while others may encourage yoga or pushing against a wall to stretch. Icing after activity. A frozen tennis ball can provide specific relief. Rolling the tennis ball under the arch of the foot after exercise can lessen pain in the area. Taping is also recommended at times. Several manufacturers of sports tape have plantar fascia specific lines. Orthotics are a good idea for those on their feet during the day. Orthotics can provide cushioning and relief. Cortisone shots in the fascia can provide temporary anti-inflammatory relief. Losing weight is perhaps the most effective method of improving heel and foot pain. Those who are overweight are far more likely to report these syndromes.
Surgical Treatment
Usually, heel spurs are curable with conservative treatment. If not, heel spurs are curable with surgery, although there is the possibility of them growing back. About 10% of those who continue to see a physician for plantar fascitis have it for more than a year. If there is limited success after approximately one year of conservative treatment, patients are often advised to have surgery.
Prevention
There are heel spur prevention methods available in order to prevent the formation of a heel spur. First, proper footwear is imperative. Old shoes or those that do not fit properly fail to absorb pressure and provide the necessary support. Shoes should provide ample cushioning through the heel and the ball of the foot, while also supporting the arch. Wearing an orthotic shoe insert is one of the best ways to stretch the plantar fascia and prevent conditions such as heel spurs. Stretching the foot and calf is also helpful in preventing damage. Athletes in particular should make sure to stretch prior to any physical activity. Stretching helps prevent heel spurs by making tissue stronger as well as more flexible. In addition, easing into a new or increasingly difficult routine should be done to help avoid strain on the heel and surrounding tissue.